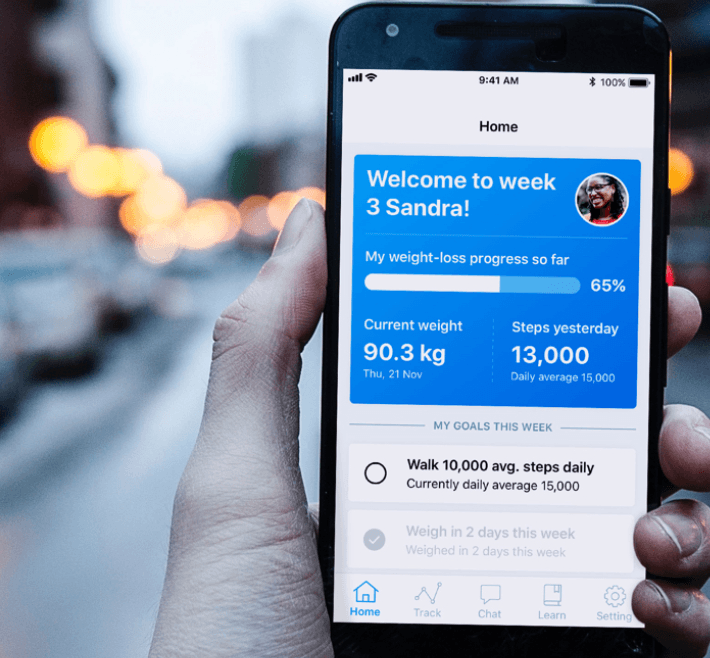
Most of the complications people suffering from Type 2 diabetes are due to a lack of awareness and understanding of the condition that are potentially preventable through healthier lifestyle choices, which can be managed with the OurPath app.
In the UK, a record number of 3.8 million people are living with a diagnosis of diabetes, and 90% of those have Type 2 diabetes, a figure that has more than doubled in the past ten years, according to research charity Diabetes UK – costing the NHS about $11bn a year.
By creating a holistic approach to behaviour change, the app-based OurPath programme has been designed to help people lead healthier lives and prevent or reduce the symptoms of the disease by addressing multiple factors impacting a user’s lifestyle.
Within a year of launching in 2016, the London-based digital health provider became the first ever online behavioural change platform to be commissioned by the NHS to support lifestyle change in diabetes treatment as part of the NHS Diabetes Prevention Programme.
Mike Gibbs, founder and chief operating officer at OurPath, said: “Upon signing up for the programme, each user will have a welcome call with their coach and so the coach will have an understanding of the needs and motivations of each user.
“Life is different for everyone so the coach and the other users in the group chat help people adapt to busy work schedules, choose dishes for dietary requirements and identify the best choice on the menu of a restaurant.
“Everyone has difficult days and the common theme is that they are looking for support to get back on course without feeling the need to return to square one – that is why incremental changes are very important.”

What is OurPath?
Health services for a long time have relied on traditional, medicinal treatments for Type 2 diabetes, a life-threatening condition that occurs when the body doesn’t produce enough insulin to function properly, or the body’s cells don’t react to insulin.
However, many healthcare organisations such as the NHS have acknowledged these solutions are no longer enough to tackle the long-term health crisis the UK faces.
In order to reduce the number of people being diagnosed with Type 2 diabetes, the common root cause needs to be addressed, which is an unhealthy lifestyle that can lead to obesity – with contributing factors including nutrition, exercise, mental wellbeing, sleep and stress.
To tackle this challenge and make lifestyle interventions more accessible to people, healthcare professionals have started to use technology as an enabler.
OurPath uses cognitive behavioural therapy to try to change how people think about their lifestyle habits, and ultimately change those behaviours to become healthier.
It partnered with pharmaceutical firm Roche, to scale up its popular coaching-based lifestyle change programme, and, as well as being privately available, OurPath is now prescribed as a Type 2 Diabetes measure in small pockets of the NHS across the UK.
A common mindset is that the use of, and reliance on, technology only makes people lazier and is overall an unfit and unhealthy method as it keep people dependent on their phones.
But Mr Gibbs told NS Medical Devices: “As the old adage goes, every medicine is a poison – technology is of course accused of being a contributing factor to less healthy lifestyles but this does not mean technology is not the answer for either individual or societal level interventions.
“There are millions of people in the UK with an increased risk of Type 2 diabetes and if we are to make a difference at scale there is no alternative to technology-based solutions.”
How does the OurPath app work to combat Type 2 diabetes?
The OurPath app is the front end of a digital service, to which people sign up when they want to change their behaviours and lead a healthier lifestyle – they can either register directly or might be referred by an NHS clinician.
Once in the app, the user is placed in a group chat with around ten others who can support one another throughout the programme.
A one-to-one chat service is also available with a personal health coach.
Those who have opted for the tech plan will receive an activity tracker and connected scales, as well as motivational advice and guidance for “rebalancing”.
“Throughout the three month programme, users are frequently alerted to new articles in the app with lifestyle tips and tricks, and receive support from their coach to navigate daily life – all of whom are real people trained as nutritionists of dietitians,” said Mr Gibbs.

“It is the key to ensuring that this tech-based service retains the human touch – from picking the best option on a restaurant menu to planning meals ahead of schedule.”
Long-term health benefits and habits are developed using the app over the three month programme as there is a focus on gradual lifestyle changes at a pace that suits the user.
The personal aspect is what makes the digital platform distinctive to other tech on the market – the coach adapts to the progress and needs of both the group and the individual to ensure no-one is left behind, and won’t shy away from pushing the user through video and text consultations to go that little bit further each week.
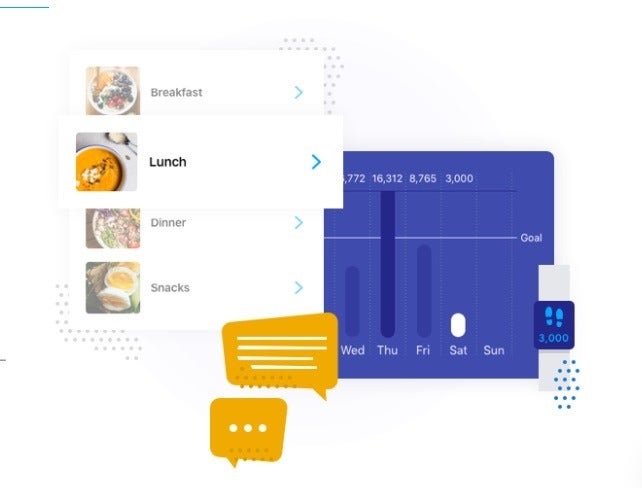
Through the app the patient can then track their progress by logging metrics such as their food intake, physical activity levels, sleep, water intake, blood sugar levels and tobacco use.
Mr Gibbs explained: “You chat to both your group members and your health coach via the app.
“There is also a strong emphasis on individual goal-setting and self-monitoring – as well as tracking weight, physical activity and food intake, all of which is done through the app.”
Towards the end of the programme, some people will feel confident enough to continue independently, but many take the opportunity to transition to the “sustain” programme, which provides ongoing access to a chat group along with other users.
“OurPath was commissioned by the North West London collaboration of CCGs over two years ago to provide our digital behavioural change programme to a population of people living with Type 2 diabetes,” added Mr Gibbs.
“This innovative pilot was the first time a digital behavioural change programme had been commissioned for the management of Type 2 diabetes.
“The NHS has set clear entry criteria for both the Healthier You: NHS Diabetes Prevention Programme, as well as any local contracts for Type 2 diabetes management, like our work in North West London.
“Having a diagnosis of Type 2 diabetes or non-diabetic hyperglycaemia [pre-diabetes] is a core referral requirement.”
What is the Healthier You: NHS Diabetes Prevention Programme?
The NHS last year launched its Healthier You: NHS Diabetes Prevention Programme, in which more than 5,000 patients are expected to benefit as five different technology companies provide digital health interventions.
The digital pilot initiative tests a range of apps, gadgets, wristbands and other innovative digital products to see their impact on people at risk of developing Type 2 diabetes.
The hope is that the programme will be rolled out nationally after the pilot to help drive healthcare efficiency and patient outcomes.






