Saving patients from undergoing invasive bypass surgeries, the use of HeartFlow’s AI-powered software by doctors in the NHS is providing them with a much clearer view of how blood is moving through the coronary arteries.
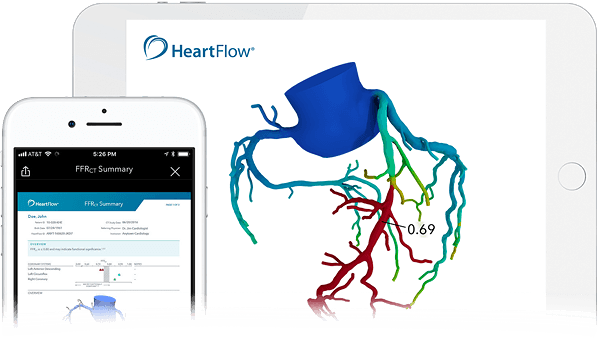
Key to both identifying and curing heart disease – the number one cause of death worldwide – the US medtech firm’s technology leverages deep learning methods and highly-trained analysts to compile CT data and create a digital, 3D model of a patient’s coronary arteries.
According to a British Heart Foundation report on heart disease and stroke statistics, approximately seven million people live with heart and circulatory disease in the UK, causing 160,000 deaths each year – an average of 435 people each day.
Dr Tim Fairbairn, the clinical lead for cardiac diagnostics at Liverpool Heart and Chest Hospital, said: “Technology like this has helped us make real steps forward when it comes to cardiovascular care.
“As recommended by the National Institute for Health and Care Excellence (NICE), a CTA-first approach is rapidly becoming the most widely used method to identify coronary arteries disease (CAD), but it is limited by the inability to tell us whether the CAD is causing the patient’s chest pain.
“The HeartFlow Analysis allows cardiologists to better determine whether the CAD is significant and causing the chest pain. For the patients themselves, it provides a less invasive and quicker overall diagnostic experience.”
How does the HeartFlow device work?
Traditional diagnostic pathways used to predict disease using blood tests involve an invasive and time-consuming process that takes several stages and can mean that life-threatening defects lead to heart failure before they can be treated.
According to Mayo Clinic, a US nonprofit academic medical centre, CAD develops when the major blood vessels that supply the heart with blood, oxygen and nutrients become damaged or diseased.
In the last decade, significant advancements in CAD treatment have come about through integrating AI, meaning monitoring the heart for life-threatening emergencies is becoming easier for all patients.
Requiring just a CT scan, HeartFlow is a test that identifies problems with blood flow, and gives doctors a prognosis of how serious the conditions might be.
Dr Fairbairn explained to NS Medical Devices: “The data from this scan is then sent securely to HeartFlow in California, via the cloud.
“The software solves millions of complex algorithms to simulate blood flow to the heart. This information helps us understand any areas where blood flow might be compromised. We’re then able to form a diagnosis and treatment plan.”
HeartFlow’s current algorithm is trained using data from almost 10,000 patients, all of which has been de-identified, preventing a person’s identity from being connected with information, and is stored locally by the hospital or practice.
How is HeartFlow working with the NHS to save $11.5m a year ?
The HeartFlow Analysis was chosen as a new technology to be funded by the Innovation and Technology Payment (ITP) programme last year, an initiative designed to accelerate the roll-out of latest technology across the UK.
The ITP designation for the HeartFlow Analysis came after NICE recommended it as the most cost-effective option, after evaluating that the use of this technology could save the NHS up to $271 per patient, equivalent to $11m a year when diagnosing CAD in patients.
Dr Fairbairn says these cost savings come from being able to avoid expensive, unnecessary procedures and focusing time in the catheterisation lab on those who really need it.

Previously, cardiologists were required to carry out angiograms – a type of X-ray coupled with dye injected into the blood vessels of the heart to detect certain risks – to achieve the same level of information the Heart Analysis provides without exploratory surgery.
He said: “While the technology doesn’t completely negate the need for invasive procedures, it offers cardiologists a much clearer view of how blood is moving through the coronary arteries.
“This often impacts the next steps taken. Studies have shown that the information produced from CT scans which have undergone the HeartFlow Analysis changed a doctor’s recommended treatment plan in two thirds of patients.
“The majority could be treated with medication only, as opposed to needing intervention like stenting or bypass surgery.”
HeartFlow is currently used in over 35 hospitals across NHS England and was recently awarded a second-round of funding under the NHS’ ITP programme.
What’s next for HeartFlow?
The team in California is currently working on a tool called HeartFlow Planner, an interactive tool that enables interventional cardiologists and heart teams to modify vessels virtually, and thereby determine the optimal treatment strategy prior to an invasive procedure.
Last month, it announced new data from a study that included 101 patients, highlighted the benefit of using its real-time interactive tool as it led to a change in treatment strategy in 45% of patients with CAD and reduced the need for invasive physiology.
“This is a real-time, non-invasive interactive planning tool that will help us to explore different treatment options by virtually modifying the cardiac blood vessels,” said Dr Fairbairn.
“It’s going through regulatory clearance at the moment but is anticipated to launch later this year.”






