
Personalised neurotechnology-aided therapy for the arm could improve recovery in severe chronic stroke patients, according to a new paper published by Switzerland-based researchers.
The common consequences observed among stroke cases is the long-term impairment or sudden paralysis of a leg, arm or one side of the face, with the resultant loss of sensation and muscle control negatively impacting quality of life.
The new study, titled Neurotechnology-aided interventions for upper limb motor rehabilitation in severe chronic stroke, illustrates how a host of therapies using techniques from robotics, brain stimulation and brain-machine interfaces can focus on treating the individual needs of patients when used in combination.
Dr Martina Coscia, staff engineer at the Wyss Center and one of the researchers, said: “Our findings show that neurotechnology-aided upper limb rehabilitation is promising for severe chronic stroke patients
“However, we also found that the ‘one size fits all’ approach doesn’t lead to the best outcome.
“We suggest a move towards a personalised combination of neurotechnology-based stroke rehabilitation therapies, ideally in a home-based environment where prolonged therapy is more feasible than in a clinic.”
How can therapy using neurotechnology help stroke patients?
Rehabilitation therapies have the largest effect in the first three months after stroke, but the severity of stroke complications and each person’s ability to recover vary widely, according to US medical advice service Mayo Clinic.
Despite some individual success stories, the reality is that most stroke patients struggle to regain the ability to speak, move around and take good care of themselves.
Often, after three months, patients are considered chronic and the likelihood of further natural recovery is limited, which is especially true for those most severely affected.
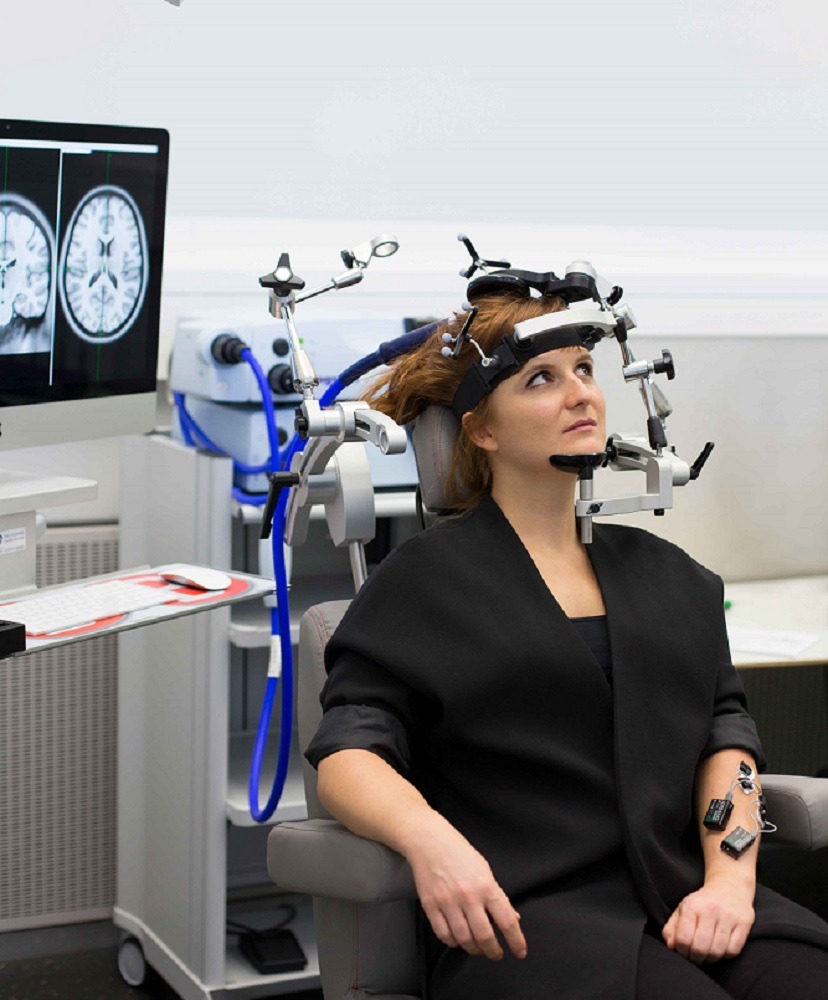
In the Wyss Center’s publication, the researchers highlight the need for longitudinal clinical studies to validate the rehabilitation effects of individual therapies and the use of multiple complementary combination therapies.
Effectiveness data from 64 cases of clinical studies based on upper limb neurotechnology treatments among stroke patients were compared by the team during the research.
The interventional technology analysed included robotics, functional electrical stimulation of muscles, brain stimulation and brain-computer interfaces – as well as their use in combination – to maximise treatment effects in each individual patient.
Based on the findings, the team believes that a synergistic approach could pave the way for new treatments.
The researchers are set to launch a clinical trial to evaluate personalised therapy, specifically intended to maximise therapy effects in individual patients.
In the long term, the aim is to build devices that help stroke survivors recover some of the functions they have lost in their arms and legs, in which “multiple neurotechnology-based therapies are used within the same patient”.
Professor Friedhelm Hummel, from the Swiss Federal Institute of Technology Lausanne (EPFL) and University of Geneva Medical School, said: “What we would like to see in the future are long-term trials in which multiple neurotechnology-based therapies are used within the same patient.
“We believe that this synergistic approach could uncover previously undiscovered treatment pathways for chronic stroke patients.”
The researchers come from the Wyss Center for Bio and Neuroengineering, the EPFL, Scuola Superiore Sant’Anna, the University of Geneva Faculty of Medicine, and the Clinique Romande de Readaptation.






