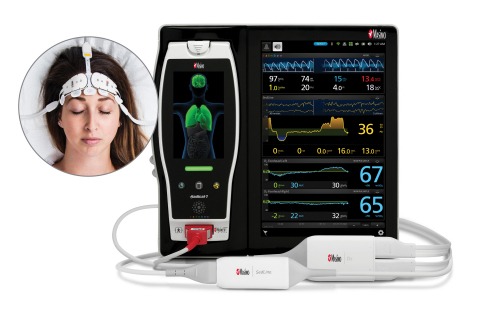
O3 uses near-infrared spectroscopy (NIRS) to monitor cerebral oxygenation in situations in which peripheral pulse oximetry alone may not be fully indicative of the oxygen in the brain.
Noting that “normative values for clinical devices are essential to allow for definition of abnormality during clinical use” and that available regional cerebral tissue oxygen saturation (SctO2) reference values have limitations, including not taking into account variables such as brain hemisphere, sex, skin type, height, weight, and others, Dr. Christopher Eyeington and colleagues used Masimo O3 to assess for differences in SctO2 between hemispheres, sex, and comorbidity and smoking status, and for associations between SctO2 and key physical and hemodynamic characteristics, in healthy adults.
They enrolled 98 volunteers, 22-60 years old, including 41 males, 22 with one or more co-morbidities, 13 current or former smokers, and with a variety of skin types. Each volunteer was monitored continuously for five minutes using O3 on the Masimo Root® Patient Monitoring and Connectivity Hub, with SctO2 measurements recorded every two seconds.
The researchers recorded 32,130 SctO2 observations. Mean left, right, and combined average SctO2 values were 67.3%, 67.9%, and 67.6%, respectively, with a “narrow” combined average 95% confidence interval of 66.8% to 68.6%. (None of the 95% confidence intervals was lower than 66.5% or greater than 69.1%.)
The researchers found “statistically significant yet quantitatively small differences” in SctO2 values according to hemisphere (p < 0.001). They also found that increasing mean arterial pressure (MAP) (p = 0.001) and cardiac index (CI) (p ≤ 0.001) were associated with increased SctO2: each 10 mmHg increase in MAP and 1 L/min/m2 increase in CI was associated with 0.01% and 0.1% increases in SctO2, respectively.
The researchers noted, “Our study implies that in healthy adults the mean SctO2 measured with modern technology is close to 68% with narrow confidence intervals of 1%, and with no difference between hemispheres. Moreover, given a lowest mean combined bi-hemispheric SctO2 value of 56%, it implies that an SctO2 value below 56% should be considered ‘abnormally low.’
“In addition, the very few SctO2 values below 60% seen in our study imply that persistent measurements below such a threshold should be viewed with concern. Finally, our observation that SctO2 values were not affected in any clinically significant amount by hemispheres, sex, skin type, comorbidity or smoking status, age or any haemodynamic parameter implies that in healthy adults, cerebral tissue oxygen saturation is unaffected by these factors.”
They concluded that “These findings have significant implications regarding the clinical interpretation of SctO2 and the application of this information to individual patients.”
Study co-author Dr. Rinaldo Bellomo commented, “The estimation of cerebral oxygenation by near infrared spectroscopy (NIRS) during anesthesia or in critical illness is becoming increasingly recognized as a desirable form of monitoring. Thus, it is vital for clinicians to understand normal values and to have confidence in the technology behind such measurements.
“The recent study by my colleagues and myself used >30,000 observations in close to 100 normal subjects and found that the mean normal value for cerebral oxygen estimation using modern Masimo NIRS technology was 67.6%, and, more importantly, that the 95% confidence interval for such value was narrow, between 66.8% and 68.6%. Such findings provide a reference value for patient assessment and give a degree of confidence to clinicians in relation to the validity and robustness of this technology.”
Source: Company Press Release






