Giving birth prematurely increases the risk of to several health conditions in a newborn, but one fairly constant implication of neonatal delivery is a lower pain threshold and the need for pain management.
The immature peripheral and central nervous systems of preterm infants mean that they’re more sensitive to pain and stress – although the two are often indistinguishable.
Despite this, pre-term babies in the NICU (neonatal intensive care unit) have to undergo an average of 10 to 12 procedures that involve breaking the skin every day, which can lead to significant pain and stress.
Currently, the standard way to manage this pain is parental touch and facilitated tucking (FT) – a technique in which babies are put into the foetal position.
The combination of these has been proven to soothe the infant, but according to Dr. Manon Ranger, a University of British Columbia (UBC) nursing professor who studies the health of vulnerable infants, the importance of this pain management goes beyond comfort.
“For newborns and particularly for preterm babies, it’s critical to keep overall blood oxygen levels steady, especially in the brain,” she said.
“The more stable their brain oxygenation is, the better for their brain development.”
Pain and stress can both contribute to changes in brain-oxygen levels, but in certain circumstances parental touch isn’t available, which is why Canadian researchers have tested a new device that could step in for the absentee carers.
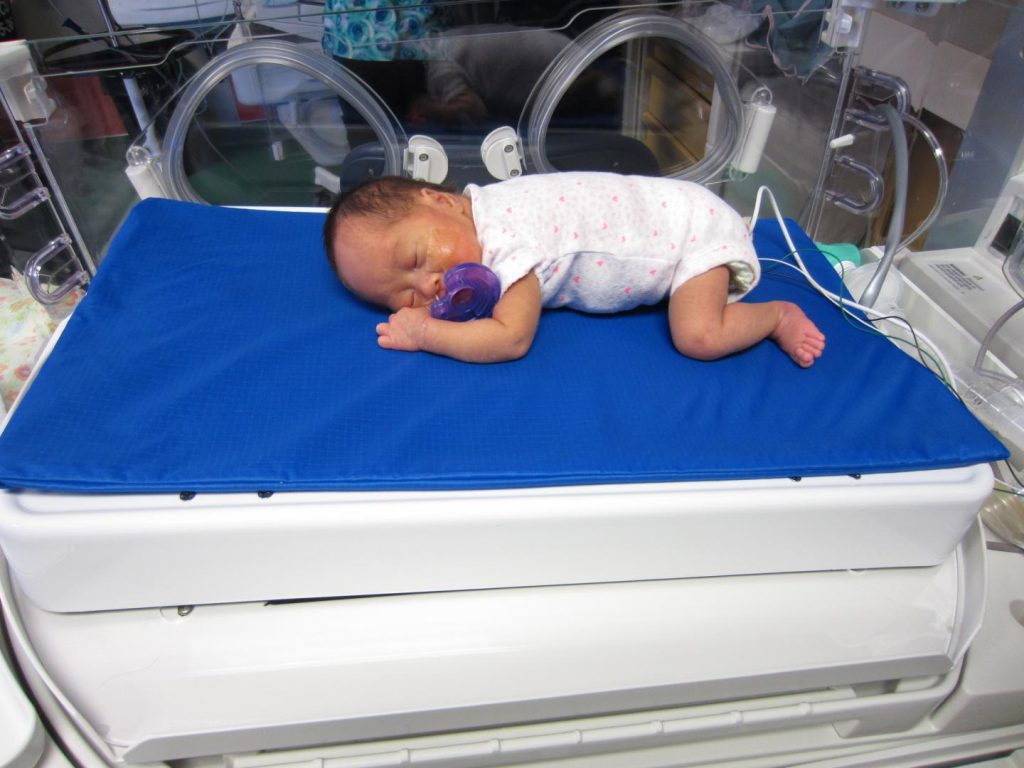
A team from the University of British Columbia, Canada, pitted Calmer, a pillow-sized therapeutic bed covered in soft fabric that can be programmed to mimic a parent’s heartbeat and breathing rate, against the standard method of parental touch and FT.
The results were published in full in the journal Pain Reports.
Calmer vs FT in neonatal pain management
The research team conducted a small randomised clinical trial with 29 premature babies admitted to the neonatal intensive care unit, or NICU, at BC Women’s Hospital and Health Centre.
Half the participants received the usual facilitated tucking while they were held and soothed by a caregiver during a painful heel lance procedure, while the other half were placed on Calmer.
When their brain oxygen levels were measured, both groups showed similar results: their brain oxygen levels stayed largely steady during the procedure.
“A parent’s touch, generally speaking, is ultimately the most soothing presence for an infant,” said Ranger, who is also an investigator at BC Children’s Hospital and Women’s Health Research Institute.
“It relieves pain, helps them gain weight and promotes brain growth while reducing stress.
“However, this option is not always available in NICUs. Our research shows that when a parent or caregiver cannot be physically present, Calmer is an effective alternative.
“This is especially relevant in the current Covid-19 pandemic context, where many hospital settings must restrict contact with visitors.”
Who developed Calmer?
Calmer was developed by Dr. Liisa Holsti, a professor in the department of occupational science and occupational therapy at UBC and Dr. Karon Maclean, a UBC professor of computer science.
Other researchers from BC Children’s Hospital, the British Columbia Institute of Technology and the BC Women’s Hospital and Health Centre also contributed to its development.
Holsti, who is also an investigator at BC Children’s Hospital and Women’s Health Research Institute, said: “We were very pleased that our preliminary trial results showed that Calmer has the potential to benefit these infants whose brains are particularly vulnerable to pain and stress.
“We are expanding our evaluation of this device in more rigorous real-world conditions, and we’re in the process of redesigning it to be used in low-and-middle-income countries, so that infants worldwide who need it can have the benefit of Calmer treatment.”
For their next step, the team is planning to test the longer-term use of Calmer on preterm infants’ physical growth and brain development in the NICU.
This project recently received funding from UBC’s Health Innovation Funding Investment (HIFI) awards.






