Cancer has long remained one of the preeminent medical threats in the world, and a diagnosis obtained early in the disease’s development through an endoscopic biopsy device can mean there’s more chance of patients going into remission.
The knock on effect of improving diagnostics is a reduction in the cost and complexity of treatment, which is why there’s no shortage of organisations looking at ways to improve detection procedures for cancers inside certain areas of the body.
Israeli firm Limaca Medical is one of these companies, and it just received $1.25m to support first-in-human procedures, post-market clinical studies, and obtain regulatory approvals for its Precision device.
“We designed Precision to improve upon endoscopic biopsies and make a substantial leap forward in this critical diagnostic procedure to advance precision treatment and achieve superior outcomes for cancer patients,” said Limaca’s CEO Assaf Klein
Limaca is a subsidiary of medical and agricultural technologies investor The Trendlines Group, which contributed to the raise alongside fellow investor Agriline and private investors that included Carl Rickenbaugh, who also holds the role of chairman within Limaca.
A veteran in the medical devices industry, Rickenbaugh believes Precision will prove itself to be superior to the standard biopsy procedures in clinical practice.
“The medical provider and payor markets respond to superior devices when they demonstrate strong clinical relevancy,” he said.
“We built Limaca to address the need for a more efficient endoscopic procedure for the provider, and for the cancer patient and payor, greater certainty to gain sufficient sample quality and quantity needed for pathology as well as more stringent genetic testing requirements.”
Limaca is currently focusing on the $850m market for pancreatic cancer diagnosis due to its five-year survival rate of 9% – the lowest of all cancers and a product of the fact that it is usually diagnosed at an advanced stage and is resistant to therapy.
The firm claims the technology can, however, also be used in the diagnosis of lung cancer, liver cancer, lymphoma and other cancers where subcutaneous tissue samplings are difficult to obtain.
These other markets the company estimates to be worth over $400 million combined.
How effective are current cancer biopsy procedures at detecting pancreatic cancer?
Although non-invasive liquid biopsies are continually improving, a tissue biopsy is still considered to be the only sampling method that can diagnose the precise histology of a tumour – the type of tissue from which it originated.
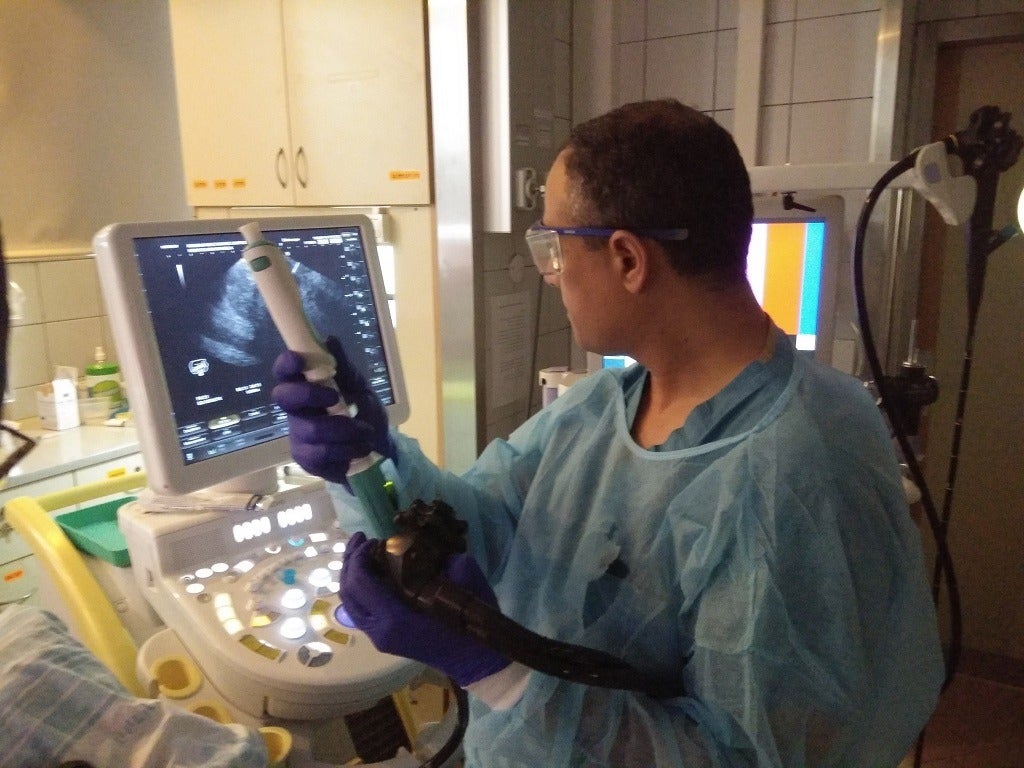
The traditional method of performing an endoscopic biopsy involves putting a flexible tube called an endoscope down the throat that contains a small ultrasound probe.
The ultrasound picture helps doctors to see any areas that might be cancerous, and they then guide a small needle into these areas to take the biopsy.
The issue with this procedure, according to Limaca, is that it provides poor tissue samples, which affect the sensitivity of diagnostic testing, and so frequently require a second go to acquire more tissue.
One meta analysis from 2016 on the use of ultrasound in combination with endoscopic biopsies (EUS) to obtain samples from pancreatic lesions suggests the method is effective, with a median 91% overall sensitivity rate determined.
But the study also found a high variance – between 73.20% and 96.50% – and although the authors suggested it could be down to differences in physician skill, it could also mean there are improvements to be made in the way clinicians conduct biopsies.
How does Limaca’s Precision improve the endoscopic biopsy procedure?
Limaca’s endoscopic biopsy device uses the same sort of design as standard biopsy equipment, but instead of a regular needle stab, it uses a rotational cutting implement.
The benefit of this adaptation, according to the company, is that samples remain intact and uncontaminated by the blood and tissue surrounding the tumour that ultimately gets picked up during the procedure.
The company also claims its Precision device requires only one pass through the GI tract and three stabs of the tumour, as opposed to what it says is an average of three passes, each requiring 10 stabs, to get enough samples for adequate diagnostic testing in a standard device.
To date, 10 patients have been enrolled in Limaca’s first-in-human study – designed to compare Limaca’s Precision to standard of care EUS biopsy devices – at the Rambam Health Care Campus in Israel.
According to Iyad Khamaysi, MD, Director, Invasive Endoscopy Unit Results at the Campus, Limaca’s device has so far “exceeded all clinical expectations for endoscopic biopsy while demonstrating clear safety.”






